World Malaria Day 2008 - Eradication is Possible!
 Friday was World Malaria Day 2008. Global health depends on controlling this global disease. It is the leading cause of death in African children and a major health concern in Haiti. It overwhelms fragile health care systems and hurts economies - the annual economic loss in Africa due to malaria is estimated to be $12 billion (1.3% loss in GDP.) Yet, we know how to prevent it and how to treat it. There has been tremendous progress made in the past year, so much so that the international community increasingly agrees that we should begin working toward eradication - in other words, a world without malaria. It would be a better world indeed.
Friday was World Malaria Day 2008. Global health depends on controlling this global disease. It is the leading cause of death in African children and a major health concern in Haiti. It overwhelms fragile health care systems and hurts economies - the annual economic loss in Africa due to malaria is estimated to be $12 billion (1.3% loss in GDP.) Yet, we know how to prevent it and how to treat it. There has been tremendous progress made in the past year, so much so that the international community increasingly agrees that we should begin working toward eradication - in other words, a world without malaria. It would be a better world indeed.
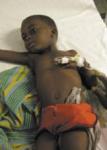 So what is malaria? Malaria is a mosquito-borne disease caused by a parasite. But not all mosquitos carry it. Only the anopheles mosquito and only the females. If you get malaria, what happens? You will likely experience fever, chills, and pain. There is a possibility you could go into a coma or develop a brain hemorrhage. At a minimum, it will be unpleasant. It could be life threatening especially if you are a child under five, a pregant women, or someone who has a compromised immunse system because of sickness or malnutrtion, both of which are in Haiti aplenty.
So what is malaria? Malaria is a mosquito-borne disease caused by a parasite. But not all mosquitos carry it. Only the anopheles mosquito and only the females. If you get malaria, what happens? You will likely experience fever, chills, and pain. There is a possibility you could go into a coma or develop a brain hemorrhage. At a minimum, it will be unpleasant. It could be life threatening especially if you are a child under five, a pregant women, or someone who has a compromised immunse system because of sickness or malnutrtion, both of which are in Haiti aplenty.
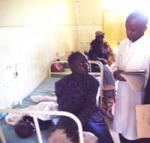 Each year 350-500 million cases of malaria occur worldwide, and over one million people die. Malaria is a disease that preys on the weak. To prevent malaria is to protect the most vulnerable members of a society.
Each year 350-500 million cases of malaria occur worldwide, and over one million people die. Malaria is a disease that preys on the weak. To prevent malaria is to protect the most vulnerable members of a society. We know how to prevent this disease and how to treat it. Let's talk about prevention first. First, an individual can sleep under a long lasting insecticide treated mosquito net. I dont call it a bed net because it assumes someone has a bed which is not always the case. This protects other members of the community as well because he or she cannot be bit by a mosquito and pass the disease on to someone else.
We know how to prevent this disease and how to treat it. Let's talk about prevention first. First, an individual can sleep under a long lasting insecticide treated mosquito net. I dont call it a bed net because it assumes someone has a bed which is not always the case. This protects other members of the community as well because he or she cannot be bit by a mosquito and pass the disease on to someone else.  Second, we can use indoor residual spraying which just means that we spray the inside of a home with an appropriate insecticide at the appropriate time of year. When mosquitos enter the home, they will die when they land on the walls.
Second, we can use indoor residual spraying which just means that we spray the inside of a home with an appropriate insecticide at the appropriate time of year. When mosquitos enter the home, they will die when they land on the walls.  Third, we can use intermittent preventive therapy which means that we give pregnant mothers doses of medication that will protect both her and her child.
Third, we can use intermittent preventive therapy which means that we give pregnant mothers doses of medication that will protect both her and her child. Fourth, we can control malaria by managing the environment - removing standing water, water run off (from waters stands for example), and trash that can collect water. Those canals in Port au Prince that collect water, pits, stagnant canals make good breeding grounds for mosquitos. Limiting locations where the vector can breed, limits the number of the mosquitos that carry the parasite.
Fourth, we can control malaria by managing the environment - removing standing water, water run off (from waters stands for example), and trash that can collect water. Those canals in Port au Prince that collect water, pits, stagnant canals make good breeding grounds for mosquitos. Limiting locations where the vector can breed, limits the number of the mosquitos that carry the parasite.
 Most of the world has become resistant to at least some of the drugs that we traditionally used to treat malaria. This has happened because of over-use, self-medication, not completing (often because of not being able to afford) the full course of treatment, counterfeit drugs, etc. Today, we have a new gold standard in artemesinin based combination therapy. It is very effective and there is little resistance to it.
Most of the world has become resistant to at least some of the drugs that we traditionally used to treat malaria. This has happened because of over-use, self-medication, not completing (often because of not being able to afford) the full course of treatment, counterfeit drugs, etc. Today, we have a new gold standard in artemesinin based combination therapy. It is very effective and there is little resistance to it.
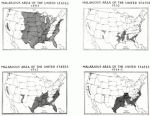 There are positive precedents for malaria control. Most of the United States used to be malaria endemic. Southern Europe used to be malaria endemic. In fact, what is now the Centers for Disease Control and Prevention (CDC) in Atlanta, was orginally founded as an institution to fight malaria in the USA. But each of these examples were from long ago. Since that time, the world has been desparate for new successes. Finally, we have them.
There are positive precedents for malaria control. Most of the United States used to be malaria endemic. Southern Europe used to be malaria endemic. In fact, what is now the Centers for Disease Control and Prevention (CDC) in Atlanta, was orginally founded as an institution to fight malaria in the USA. But each of these examples were from long ago. Since that time, the world has been desparate for new successes. Finally, we have them.

 Ethiopia and Rwanda have become the first "high burden" countries to, using the tools above, reduce their malaria mortality nationwide by 50%. This is historic - it has never happened before. Neither of this countries is rich in resources but they had the will, a plan, and the support of the international community. It did not take long to see the impact. For example, in Ethiopia the drugs and nets were introduced in 2005. Hospitalized malaria cases in young children fell 60 percent and deaths 51 percent by 2007. Presure on the health care system was alleviated and many young lives were saved. If it can happen in Rwanda and Ethiopia, it can happen in Haiti as well.
Ethiopia and Rwanda have become the first "high burden" countries to, using the tools above, reduce their malaria mortality nationwide by 50%. This is historic - it has never happened before. Neither of this countries is rich in resources but they had the will, a plan, and the support of the international community. It did not take long to see the impact. For example, in Ethiopia the drugs and nets were introduced in 2005. Hospitalized malaria cases in young children fell 60 percent and deaths 51 percent by 2007. Presure on the health care system was alleviated and many young lives were saved. If it can happen in Rwanda and Ethiopia, it can happen in Haiti as well.
There is a sense of hope and growing optimism among those who fight against malaria whether they be doctors, public health specialists, administrators, or researchers that we are finally making progress and gaining ground against one of humankinds oldest foes. What has changed?
 First, the United States is throwing its clout and resources into fighting malaria. Announced in June 2005, the President's Malaria Initiative (PMI) combined the technical expertise and resources of the United States Agency for International Development, the Centers for Disease Control and Prevention, and a wide network of non governmental organizations and faith based groups. The PMI works both at the grasroots to ensure communities have ownership over malaria programming and with the host government to ensure they have the capacity to carry on the fight against malaria over the long haul. The PMI is focusing its activities in Angola, Benin, Ethiopia, Ghana, Kenya, Liberia, Madagascar, Malawi, Mali, Mozambique, Rwanda, Senegal, Tanzania, Uganda, and Zambia. It plans to spend $1.2 billion between 2005 and 2010.
First, the United States is throwing its clout and resources into fighting malaria. Announced in June 2005, the President's Malaria Initiative (PMI) combined the technical expertise and resources of the United States Agency for International Development, the Centers for Disease Control and Prevention, and a wide network of non governmental organizations and faith based groups. The PMI works both at the grasroots to ensure communities have ownership over malaria programming and with the host government to ensure they have the capacity to carry on the fight against malaria over the long haul. The PMI is focusing its activities in Angola, Benin, Ethiopia, Ghana, Kenya, Liberia, Madagascar, Malawi, Mali, Mozambique, Rwanda, Senegal, Tanzania, Uganda, and Zambia. It plans to spend $1.2 billion between 2005 and 2010.

The establisment of the Global Fund to Fight HIV/AIDS, Tuberculosis, and Malaria in 2002 was another landmark. The Fund is a multilateral partnership between governments, civil society, the private sector and affected communities. The Global Fund's purpose is to attract, manage and disburse resources to fight AIDS, TB and malaria. The fund does not implement programs - instead they make the programs possible with their support. Since its founding in 2002, the fund has provided $3.6 billion for malaria programs. The United States is by far the largest donor to the Global Fund. Click here to see the Fund's statistics on HIV/AIDS, TB, and malaria in Haiti. Click here to see which organizaions are being receiving support for HIV/AIDS, TB, and malaria programming through the Global Fund.
 The support of the PMI and the Global Fund is very important. The World Health Organization (WHO) estimates that about $4.5 billion a year is needed to control and treat the disease. At the moment, about $1 billion is spent yearly by donor countries and about $600 million by countries where malaria is prevalent. The insecticide-treated nets can cost up to $5.50 each plus the cost of distributing them. However, now the nets are being produced in Africa. Depending on how they are purchased, the ACTs can run between one and three dollars. This does not seem like a lot to save a life, but when you are making less than a dollar a day the cost can be prohibitive.
The support of the PMI and the Global Fund is very important. The World Health Organization (WHO) estimates that about $4.5 billion a year is needed to control and treat the disease. At the moment, about $1 billion is spent yearly by donor countries and about $600 million by countries where malaria is prevalent. The insecticide-treated nets can cost up to $5.50 each plus the cost of distributing them. However, now the nets are being produced in Africa. Depending on how they are purchased, the ACTs can run between one and three dollars. This does not seem like a lot to save a life, but when you are making less than a dollar a day the cost can be prohibitive.
 Non governmental organizations are showing a renewed sense of committment as well. The New York based group Malaria No More is a network of very different organizations that all share a goal - to reduce sickness and death from Malaria. Malaria No More works to raise the profile of the disease among the public, policymakers, and businesses, while engaging the private sector to provide life-saving nets and other critical interventions. Want to be involved? Click here to find a fundraising toolkit and other resources that will be useful to you. For teachers, there is also a very accesible module on educating children about malaria. If you prefer to make a direct donation so the Network can purchase mosquito nets, click here.
Non governmental organizations are showing a renewed sense of committment as well. The New York based group Malaria No More is a network of very different organizations that all share a goal - to reduce sickness and death from Malaria. Malaria No More works to raise the profile of the disease among the public, policymakers, and businesses, while engaging the private sector to provide life-saving nets and other critical interventions. Want to be involved? Click here to find a fundraising toolkit and other resources that will be useful to you. For teachers, there is also a very accesible module on educating children about malaria. If you prefer to make a direct donation so the Network can purchase mosquito nets, click here.
 Take a look as well at the Nothing But Nets Campaign. Nothing But Nets is a grassroots campaign to save lives by preventing malaria. This initiative was kicked off with a column that Rick Reilly wrote about malaria in Sports Illustrated. He challenged each of his readers to donate at least $10 for the purchase of nets. The response was incredible and led to the creation of a campaign. Want to help but don't know where to get started? Nothing But Nets makes it easy - click here to learn how. Involve your office, your church, or any other organizations you are involved. Make a difference and have fun at the same time! Also, take a look at their "Deliver the Net" online game. If you complete the game, a net will be donated by a corporate sponsor.
Take a look as well at the Nothing But Nets Campaign. Nothing But Nets is a grassroots campaign to save lives by preventing malaria. This initiative was kicked off with a column that Rick Reilly wrote about malaria in Sports Illustrated. He challenged each of his readers to donate at least $10 for the purchase of nets. The response was incredible and led to the creation of a campaign. Want to help but don't know where to get started? Nothing But Nets makes it easy - click here to learn how. Involve your office, your church, or any other organizations you are involved. Make a difference and have fun at the same time! Also, take a look at their "Deliver the Net" online game. If you complete the game, a net will be donated by a corporate sponsor.
 The UN Secretary General Ban Ki Moon has urged the world to increase their committment to fighting malaria. Ban and his special envoy for malaria, Ray Chambers, said they wanted all African countries to have enough mosquito nets or quality household sprays for the entire population by December 31, 2010 along with sufficient malaria clinics and preventative treatment centers for high-risk pregnant women. This is both ambitious and welcome. We need to set out sights high. Earlier this month, the WHO said climate change may exacerbate health crises, including malaria, in many countries already strained by inadequate hospitals, too few medical staff and uneven access to drugs.
The UN Secretary General Ban Ki Moon has urged the world to increase their committment to fighting malaria. Ban and his special envoy for malaria, Ray Chambers, said they wanted all African countries to have enough mosquito nets or quality household sprays for the entire population by December 31, 2010 along with sufficient malaria clinics and preventative treatment centers for high-risk pregnant women. This is both ambitious and welcome. We need to set out sights high. Earlier this month, the WHO said climate change may exacerbate health crises, including malaria, in many countries already strained by inadequate hospitals, too few medical staff and uneven access to drugs.
 The United Nations Childrens Fund (UNICEF) is the world’s largest global procurer and deliverer of insecticide-treated nets (over 18.8 million in 2007.) UNICEF states that it is on the ground in over 150 countries and territories to help children survive and thrive, from early childhood through adolescence. UNICEF is funded entirely by the voluntary contributions of individuals, businesses, foundations and governments. Click here to read a press release about UNICEF's committment to fighting malaria.
The United Nations Childrens Fund (UNICEF) is the world’s largest global procurer and deliverer of insecticide-treated nets (over 18.8 million in 2007.) UNICEF states that it is on the ground in over 150 countries and territories to help children survive and thrive, from early childhood through adolescence. UNICEF is funded entirely by the voluntary contributions of individuals, businesses, foundations and governments. Click here to read a press release about UNICEF's committment to fighting malaria.
 Also I wanted to mention the Measles Initiative, which is also helping in the fight against malaria. The Measles Initiative was formed in 2001 as a partnership between the American Red Cross, UNICEF, the WHO, the United Nations Foundation, and the CDC. Numerous other stakeholders from Academia, the private sector, and faith based organizations have since joined. Since 2001, the Measles Initiative has supported campaigns in more than 50 countries and the results have been impressive. Global mortality from measles has declined 68% with the largest reduction taking place in Africa where it has declined 91%. Why mention the Measles Initiative? 84% of measles campaigns included at least one other intervention such as mosquito net distribution, deworming, etc.
Also I wanted to mention the Measles Initiative, which is also helping in the fight against malaria. The Measles Initiative was formed in 2001 as a partnership between the American Red Cross, UNICEF, the WHO, the United Nations Foundation, and the CDC. Numerous other stakeholders from Academia, the private sector, and faith based organizations have since joined. Since 2001, the Measles Initiative has supported campaigns in more than 50 countries and the results have been impressive. Global mortality from measles has declined 68% with the largest reduction taking place in Africa where it has declined 91%. Why mention the Measles Initiative? 84% of measles campaigns included at least one other intervention such as mosquito net distribution, deworming, etc.
 A resource you might also find useful is the Roll Back Malaria (RBM) Partnership, launched in 1998 by the WHO, UNICEF, UNDP, and the World Bank. Partners include malara endemic countries, international organziations, foundations, non governmental organizations, private sector companies and academic institutions. The purpose of the partnership is to increase investments in malaria, facilitate collaboration, and to advocate for change at community, national, regional, and global levels.
A resource you might also find useful is the Roll Back Malaria (RBM) Partnership, launched in 1998 by the WHO, UNICEF, UNDP, and the World Bank. Partners include malara endemic countries, international organziations, foundations, non governmental organizations, private sector companies and academic institutions. The purpose of the partnership is to increase investments in malaria, facilitate collaboration, and to advocate for change at community, national, regional, and global levels.
A malaria vaccine is not close. Only one vaccinate candidate is even ready for the expensive, time consuming and absolutley necessary clinical trials which will indicate whether it is safe and effective. Another may be ready in a year or so. This is not an excuse to be passive. Based on the experiences of Rwanda, Ethiopia, and other countries we know we have the knowledge and the tools. Increasingly, we have the political will and the resources as well. Experience in Africa teach us what Haiti needs - political will, a plan, leadership by the government and the involvement of communities. A malaria free Haiti will be stronger, healthier, and more prosperous. It can be done!
Bryan
Add new comment